Cat Vaccinations
When it comes to medicine, there is no “one-size-fits-all” approach. And preventive care recommendations for our cats are no exception.
Cat vaccination recommendations are among the most contentious debates in veterinary medicine. It’s easy to be overwhelmed when you hear conflicting information about whether your cat needs them and the adverse effects they may have.
Even though it’s a confusing topic, making sure your cat has the shots they need and keeping up with booster shots is very important.
Cat Vaccination Guidelines and Standards
The Feline Vaccination Advisory Panel regularly evaluates and researches cat vaccination developments to make science-based recommendations. The panel comprises dedicated feline veterinarians and scientists and is regarded as a reputable source of cat vaccination standards.
Their guidelines, published by the American Association of Feline Practitioners, are among the most trusted and utilized recommendations in the field.
They divide cat vaccines into two categories:
- Core vaccines (highly recommended by most vets)
- Noncore / lifestyle vaccines (sometimes recommended by your vet)
Core vaccines are those recommended for all cats, no matter where they live or under what conditions. Vaccines that are appropriate for some cats in some circumstances are considered noncore vaccines (or lifestyle vaccines).
What Vaccines Should My Cat Get?
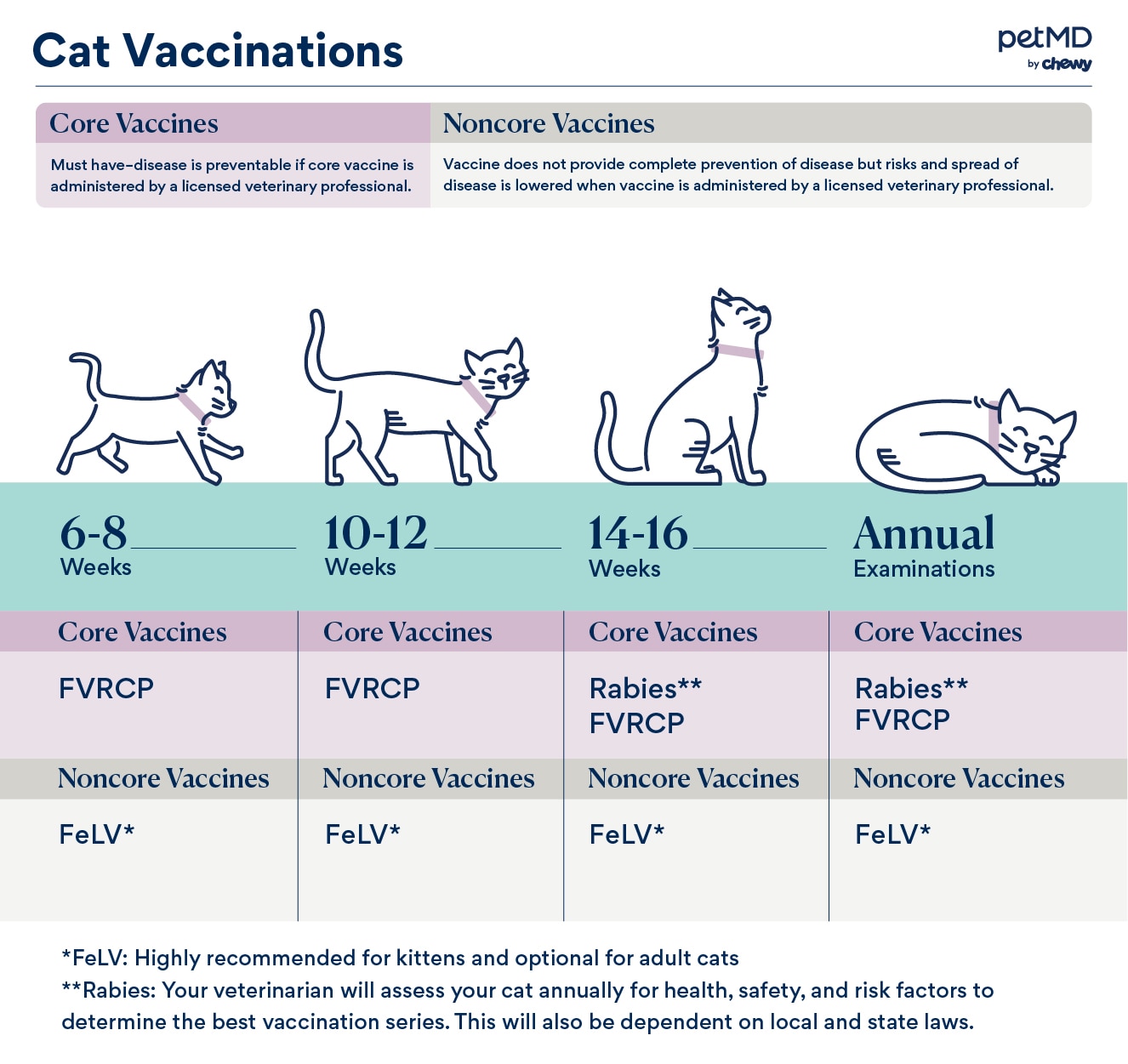
Most vets will highly recommend the FVRCP and rabies vaccines. These diseases are highly infectious and seen worldwide. They are very dangerous to young cats, and the vaccines are considered to provide a good deal of protection with minimal risk.
The FeLV vaccine is tricky because it is required for kittens but optional for cats that are at least a year old.
Rabies Vaccine (Core)
Rabies vaccination is given every year or every three years, depending on state laws and the brand of vaccine used.
Rabies is significant not only for its effect on the cat but because it is a disease that is transmissible to humans and can be fatal.
While cats are not natural carriers for the disease, they can be infected by a bite from any infected mammal and then pass it on to others. After an incubation stage, clinical signs of aggression, disorientation, and death rapidly progress.
Rabies is endemic worldwide, and the vaccine is recommended for all pet cats.
While the rabies vaccine is not listed as a core vaccine by the AAFP guidelines, it is required by law in most regions. Rabies is a zoonotic disease (it can be transmitted from animals to humans), so it is a public safety issue to keep your cat up to date on their rabies vaccine.
FVRCP Vaccine (Core)
The other three core vaccines are combined into a single three-in-one vaccine called the FVRCP vaccine. This allows veterinarians to efficiently administer the vaccines all at once, instead of having to inject a cat three separate times in one visit:
- Feline rhinotracheitis virus/herpesvirus 1 (FVR/FHV-1)
- Feline Calicivirus (FCV)
- Feline Panleukopenia (FPV)
If your cat is an indoor adult cat, FVRCP can be done every three years. If they are outdoor or indoor/outdoor, or they are young cats or seniors, your vet may recommend yearly FVRCP shots.
Cats heading into stressful situations, such as boarding, may benefit from a core vaccine booster 7-10 days before.
Feline Panleukopenia - FPV
Feline panleukopenia, also known as feline parvovirus, is a highly infectious disease with a high mortality rate in kittens.
While the disease usually starts with decreased energy and low appetite, it progresses to vomiting and diarrhea. The virus also kills off white blood cells, leaving the young cats even more susceptible to secondary infections.
Feline Rhinotracheitis Virus/Herpesvirus 1 - (FVR/FHV-1)
Feline herpesvirus, also known as feline rhinotracheitis virus, causes severe signs of upper respiratory infection.
Some symptoms you can expect to see include sneezing, nasal congestion and discharge, and conjunctivitis. In some cases, it also causes oral ulceration and pneumonia.
After the cat recovers from the initial infection, the virus enters a latency period in the nerves. During times of stress, the virus can reactivate, and the cat can start to show signs of infection again—even if they have not been re-exposed to the disease.
Feline Calicivirus - FCV
Feline calicivirus encompasses a number of viral strains that cause signs of upper respiratory infection, such as sneezing and nasal discharge as well as oral ulcerations.
FCV is thought to be associated with chronic gingivitis/stomatitis, a very painful inflammation of the gums and teeth. Some of the more virulent strains cause hair loss and crusting on other parts of the body, as well as hepatitis and even death.
FeLV Vaccine (Core for Kittens)
The FeLV vaccine works to protect your cat against feline leukemia virus.
FeLV is found worldwide. Transmitted through body fluids including saliva, urine, and feces, FeLV is spread when an infected cat comes into close contact with another cat that they groom or share bowls with.
Infection with FeLV is not an automatic death sentence. Many cats are fortunate to go into a regressive state and appear perfectly healthy throughout their lives, but some do not fare as well.
After a latent period lasting months or even years, the disease often progresses to a variety of associated conditions: lymphoma, anemia, or immunosuppression resulting in secondary disease.
The FeLV vaccine is recommended as core for kittens. The initial vaccination series consists of two doses spaced three to four weeks apart, followed by revaccination one year later for all adult cats.
However, based on most recent data, the Vaccine Advisory Panel recommends that subsequent vaccines may be administered based on risk: yearly for high-risk cats, and every two years for lower-risk cats.
Your veterinarian can assess your cat’s risk of FeLV infection and decide on an appropriate vaccination schedule.
Cat Vaccination Schedule
Many factors affect the likelihood of a cat developing an infectious disease. The factors that your veterinarian will consider to determine your cat’s vaccination schedule include:
- Age
- Medical history
- Vaccination history
- How likely they are to be exposed to a pathogen
- Severity of disease caused by a pathogen
- State laws
- Brand of vaccine
Discuss your cat’s lifestyle and risk factors with your veterinarian to determine an optimal, individualized vaccination protocol.
Here are the general cat vaccination guidelines to use as a starting point:
Kittens (up to 1 year of age)
- 6-8 weeks:
- FVRCP (core)
- FeLV (core)
- 10-12 weeks:
- FVRCP (core; first or second shot)
- FeLV (core; first or second shot)
- 14-16 weeks:
- FVRCP (core; only if first shot given at 10-12 weeks)
- Rabies
- FeLV (core; only if first shot given at 10-12 weeks)
- 1 year after initial series:
- FVRCP booster
- Rabies booster
Adult and Senior Cats (Over 1 year old)
- Every year:
- FELV (optional non-core vaccine)
- Every 1-3 years:
- FVRCP (every 3 years for indoor cats, and every year for indoor/outdoor, outdoor-only, very young, or senior cats)
- Rabies (1-year or 3-year vaccine depending on state laws)
Featured Image: iStock.com/MightyPics
